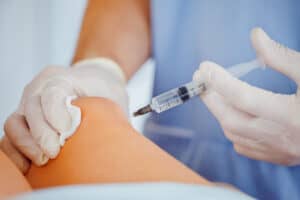
The use of injection therapy in workers’ compensation is a growing trend that is being used for a variety of injuries. This includes primarily injuries to joints such as knees, elbows, and hips. It also has practical applications for other injuries involving claims to the back and neck. Members of the claim management team should be aware of emerging trends to better manage claims.
Understanding Common Injection Therapies
Therapy injections are injected directly into a joint or tissue with a local antithetic. This procedure is primarily performed primarily in a clinical setting. It can be performed by a doctor, or other mid-level practitioner such as physician assistant, nurse practitioner, and other approved clinical officer.
Click Link to Access Free PDF Download
“The 6-Step Process To Determine Workers’ Comp Injury Causation”
Common injections include:
- Corticosteroids such as general steroids, or cortisone, which is a mixture of medications used to reduce inflammation in tissue. They are rather inexpensive and generally cost about $50 to $200 per injection; or
- Viscosupplmentation injections such as Hyaluronic Acid, which is found in human cartilage. These injections serve as a lubricant or shock absorber and are frequently used to reduce pain in patients suffering from arthritis and osteoarthrosis. They are performed in a series of injections, usually sets of three, and on a weekly basis. These injections are more expensive, and generally cost around $1,200 to $1,500 for the series.
Work Comp Injuries Involving Injection Therapies
There are a variety of instances where the use of injection therapy to cure and relieve the effects of a work injury has a common application. You will find this therapy being recommended in instances that involve:
- Knee or other joint arthritis;
- Lateral epicondylitis (tennis elbow);
- AC joint osteoarthritis;
- Carpal tunnel syndrome or de Quervain’s Syndrome;
- Hip impingement syndrome;
- Trigger finger; or
- Plantar fasciitis.
They are also commonly used in back injuries involving spinal stenosis, or disc herniations. The most common uses for therapeutic injections in workers’ compensation claims involve:
- Meniscus tears: The meniscus serves as the padding or “cushion” in the knee. Changes occur through an acute injury (twisting or pivoting motions) or degenerative changes caused by repeated movements over a period of time. In some instances, injections to the knee are not recommended given its location inside the joint. However, it can provide effective conservative care that prolongs the need for surgery and minimizes pain and swelling; and
- Rotator cuff tears: Inflammation in the shoulder’s bursa and rotator cuff tendons are common sources of problems in workers’ compensation claims. Movement of the shoulder only adds to issues. Injections that are combined with physical therapy should be a standard protocol as surgical intervention can be costly, in terms of medical expenses and times lost from work.
Tips for Effective Claim Management
The claim handler needs to be aware of how injection therapy is used, and when it is reasonable and necessary. Proactive members should be aware of the following before admitting injuries outlined above, or authorizing this form of treatment:
- Ask detailed questions regarding the mechanism of injury. When in doubt, consult with a medical director, or defense attorney who has an understanding of these type of claims;
- Review all relevant medical records associated with the claim. The injured employee should have unsuccessfully completed other treatment modalities before undergoing therapeutic injections. Any medical provider recommending therapeutic injections must provide a reasonable justification for the procedure(s);
- Requests for therapeutic injections in “off label” situations can present a number of issues. This is something that should be escalated to a claim manager or roundtable discussion; and
- Understand therapeutic injections can be an effective form of conservative care when performed in the correct manner. They can often be used in conjunction with physical therapy to providing lasting, long-term relief. It can also be used to avoid the need for more expensive and invasive procedures such as surgery.
Conclusions
Therapeutic injections can serve as effective medical care and treatment for a variety of work injuries. It is important for claim handlers to understand the mechanism of injury, prior medical care, and medical justification before approving this treatment modality. Failure to do so can result in unnecessary litigation, and prolonged medical care and disability.

Author Michael Stack, CEO Amaxx LLC. He is an expert in workers’ compensation cost containment systems and helps employers reduce their workers’ comp costs by 20% to 50%. He works as a consultant to large and mid-market clients, is a co-author of Your Ultimate Guide To Mastering Workers Comp Costs, a comprehensive step-by-step manual of cost containment strategies based on hands-on field experience, and is founder & lead trainer of Amaxx Workers’ Comp Training Center .
Contact: mstack@reduceyourworkerscomp.com.
Workers’ Comp Roundup Blog: https://blog.reduceyourworkerscomp.com/
©2019 Amaxx LLC. All rights reserved under International Copyright Law.
Do not use this information without independent verification. All state laws vary. You should consult with your insurance broker, attorney, or qualified professional.