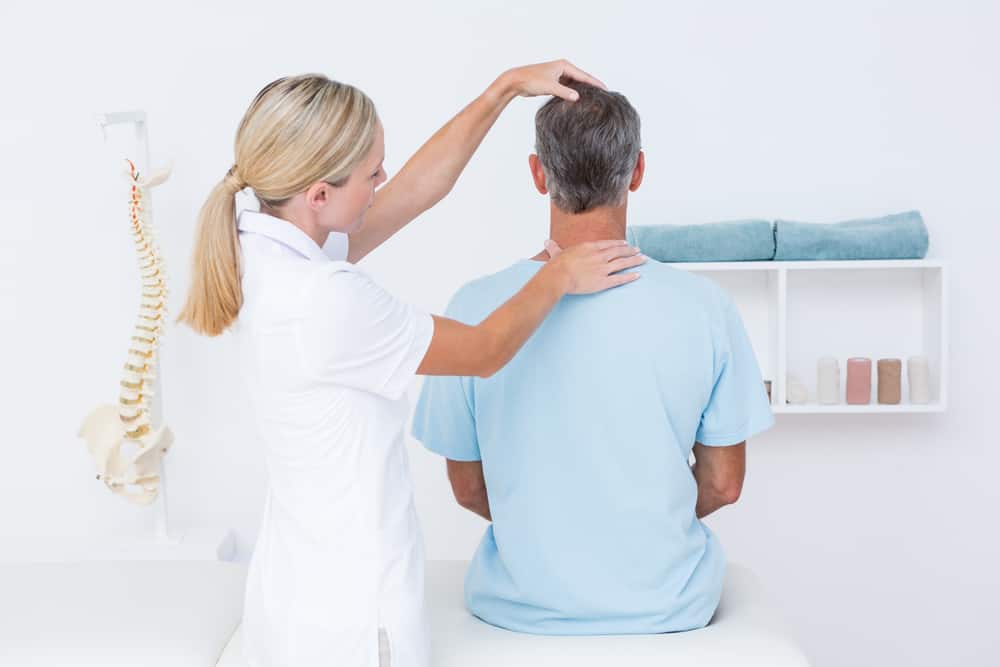
Six Ways An Employer Can Dispute Ongoing Medical Workers Compensation Treatment(s).
- Medical Treatment Plan Non-Compliance
Usually non-complianceby the injured employee in following the treatment plan is, in some aspect, covered in all states.
Claimants can end up losing their medical coverage for their claim when they
- Miss scheduled medical appointments.
- Often reschedule appointments.
- Miss or reschedule physical therapy dates.
- Treat for their condition using non-conventional methods.
They may get coverage back when they are compliant with the treatment plan and treat when and where they are supposed to.
Click Link to Access Free PDF Download
“The 6-Step Process To Determine Workers’ Comp Injury Causation”
Some claimants try these tactics in an attempt to extend the life of the claim, especially when return-to-work is looming and they do not want to go back. Discuss with your adjuster/carrier those defenses in place to prevent this scenario for happening.
- The Physician Does Not Properly Notate the Medical Chart
Chiropractors,unfortunately, seem to fail in this category. Some (not all) do not even keep an actual medical chart with notes. Sometimes they briefly chart pain complaints and indicate pain progress. Overall, the notes are not detailed and fail to show medical improvement (progression).
Physicians must keep detailed notes showing objective and subjective complaints, and the causal relation back to the injury. They must do this to properly treat their workers compensation patients. Without this crucial information, you, the employer, will not know what is being treated, how treatment correlates back to the workplace injury, and what progress the worker is making toward full recovery and returning to work.
- The Physician’s Office Ignores Adjuster Requests for Information
Adjusters often faxa request or call the treating doctor asking for answers to specific questions or for medical notes. Every doctor’s office is different, but at times weeks, even months, can go by and the adjuster will still be waiting for the doctor to address their questions.
When this happens, (depending on jurisdiction) further treatment may be suspended since requests for information pertinent to the claim are being ignored by the physician. Lack of physician response happens especially when an adjuster asks a physician to address the causal relation of the injury to the medical evidence found on exam. Sometimes doctors don’t want to address this question because they fear involvement in a potential lawsuit. Doctors feel their job is to treat the patient regardless of the complaints or how the injury occurred in the first place. Your adjuster knows what defenses you may employ, usually this is the time for an Independent Medical Evaluation (IME) to clarify medical issues.
-
Claimants Treat with the Incorrect Physician Specialty for Their Injury
If a worker has a basic laceration with sutures, there is no need to see a chiropractor, acupuncturist, or psychologist. As straightforward as this seems, surprisingly, in states where patients have the freedom to seek treatment with whomever they want, incorrect and inappropriate treatment options are frequently selected. Look at inappropriate treatment choices making no medical sense as a warning sign and “assume” something bizarre is going on.
- Physicians Do Not Discharge the Patient After Reaching End-of-Healing
Sometimes doctorsask to see patients two to three months following discharge of patients to regular duty as a follow up on their treatment. Depending on the injury, a follow up may be appropriate.
However, using our laceration as an example, a doctor wanting to see the worker five times after discharge is fishy. Physical therapists can be guilty of this charge. The doctor releases the patient to full duty without restrictions, but the therapist recommends more treatment and tries to get away with more unneeded therapy. If this is going on, intervene and ask the physician why the treatment is going on and how this relates to the injury and return to work status. It is important to work with a reputable physical therapy and rehab network.
- Claimants Try to Treat After They Have Been Discharged By an IME
An independent medicalexam (IME) is one of the adjusters best tools. Adjusters usually send patients for an IME because something is not adding up medically. Either the treatment is going on a lot longer than expected, or something in the medical notes does not make sense. Typically, claimants tell the doctor they have tons of symptoms, and the physician’s job should be to sort out what is work-related, what is not, and what makes no medical sense. Oftentimes, the doctor mentions allegations only to ignore them, and does not discharge patients when their subjective complaints do not match their objective signs of evidence.
In spite of an IME releasing a claimant to full duty and advising no further treatment is needed, the patient sometimes tries to return to the original physician for more treatment. Most states have good defenses for the insurance company in these scenarios and most times you are well-protected. However, it is always a good idea to follow up with your adjuster to stay on top of the file. Keeping up is especially important if certain forms have to be filed with the state in order to exempt ongoing treatment from coverage under workers compensation benefits.
Every state is different, and it is very important to clarify with your carrier or adjuster which laws apply in both your state and your circumstances. Employers must be aware even though workers may be released to full duty or may not have a severe injury, they may still try to get away with a lot medically. Treatments beyond medical necessity will increase both the costs and extend the life of your claims. If you remain vigilant and know what defenses are at your disposal, you can remain proactive and aggressive in making sure injured workers receive appropriate treatment, with the proper physician, for the right amount of time.
Author Rebecca Shafer, JD, President of Amaxx Risks Solutions, Inc. is a national expert in the field of workers compensation. She is a writer, speaker, and website publisher. Her expertise is working with employers to reduce workers compensation costs, and her clients include airlines, healthcare, printing/publishing, pharmaceuticals, retail, hospitality, and manufacturing. See www.LowerWC.com for more information. Contact: RShafer@ReduceYourWorkersComp.com
WORK COMP CALCULATOR: http://www.LowerWC.com/calculator.php
MODIFIED DUTY CALCULATOR: http://www.LowerWC.com/transitional-duty-cost-calculator.php
WC GROUP: http://www.linkedin.com/groups?homeNewMember=&gid=1922050/
SUBSCRIBE: Workers Comp Resource Center Newsletter
Do not use this information without independent verification. All state laws vary. You should consult with your insurance broker or agent about workers comp issues.
©2011 Amaxx Risk Solutions, Inc. All rights reserved under International Copyright Law. If you would like permission to reprint this material, contact Info@ReduceYourWorkersComp.com